COVID Testing: What is the Best Choice?

As we are entering the eighth month of the COVID-19 pandemic in the United States, pandemic fatigue can become a real concern. As a society, we can become lax in our vigilance to maintain proper health and safety standards. However, simple preventative measures like handwashing and social distancing, in addition to accurate COVID testing, are all important steps in slowing the spread as we wait for an effective vaccine to be developed.
As you know, social distancing, wearing masks, handwashing, and self-quarantining are things we can do within our own abilities and resources, but getting accurately tested for COVID-19 remains just outside of the window of self-care. With so many places to go, and multiple types of tests available, how do we know which test is the right test, and when? The answer to these questions are directly related to your personal preference and priorities. These include how accurate you want the test to be, how quickly you want to receive the results, and what level of discomfort you are willing to endure in order for the test to be taken.
There are three types of tests available: molecular, antigen, and antibody. And there are three different ways to acquire a sample for testing: spitting into a collection device, a deep nasal swab, or extraction of blood intravenously. Each one of these tests have their advantages and disadvantages based on accuracy, price, and method of sampling. We will cover these differences below to help you make the best decision for you.
Am I Currently Infected?
If you are experiencing symptoms or have been around somebody who has been diagnosed with COVID-19, there are two types of diagnostic tests you can take: molecular tests, and antigen tests.
Molecular Tests (also called PCR tests, viral RNA tests, or nucleic acid tests)
These tests can be administered in multiple ways including nasal swabs, throat swabs, and tests of saliva or other bodily fluids.
This type of test can be performed at a hospital, clinic, or other medical type office either in the facility or while you wait in your car. You can even have qualified technicians test you at home or at your place of business.
Molecular tests look for specific genetic material (ribonucleic acid or RNA) that comes only from the virus.
Molecular testing is the most accurate diagnostic test delivering both a very low rate (as low as 2%) of false negatives – which is a test result that says you don’t have the virus when you actually do have it – and a near-zero rate of false positives – that is, a test that says you have the virus when you actually do not. Molecular tests are rated by the FDA at 99% accurate and many travel restrictions require a molecular test be conducted prior to arrival.
A molecular test, using a deep nasal swab, is usually the best option due to its accuracy rate however this can be fairly uncomfortable. Other diagnostic sampling methods like throat swabs or saliva are available but can produce less accurate results.
Depending on lab capacity, results from molecular testing may be available the same day. However, there are only a few labs that process molecular testing, so additional time to ship the sample to a certified lab as well as heavy testing times can extend the time it takes for you to get your results. The Molecular RT-PCR test is the gold standard of COVID-19 testing, and it is for that reason that Pro Safety & Rescue (a CLIA certified laboratory) has invested in providing you with the best testing in the shortest time possible.
Antigen Test (also called Rapid Test)
These tests are also done through nasal or throat swabs, however, require longer time inside the nasal cavity of the patient which can greatly increase discomfort.
Just like with molecular testing, antigen tests are performed at hospitals, clinics, inside your car, or even in your home or workplace through concierge medical services.
Antigen tests identify protein fragments (antigens) from the virus that trigger the body’s immune system.
The reported rate of false negatives is as high as 50%. This can be attributed to testing too early as there is not yet a detectable level of antigens present even though the virus itself is present. The graph below shows the time the virus has entered the patient to when the antigens are detectable. This can be as high as four to five days. Any test administered during this time would show as negative, even though the patient, in fact, is positively infected with the virus. A molecular test, however, can detect COVID-19 RNA even while the patient is asymptomatic.
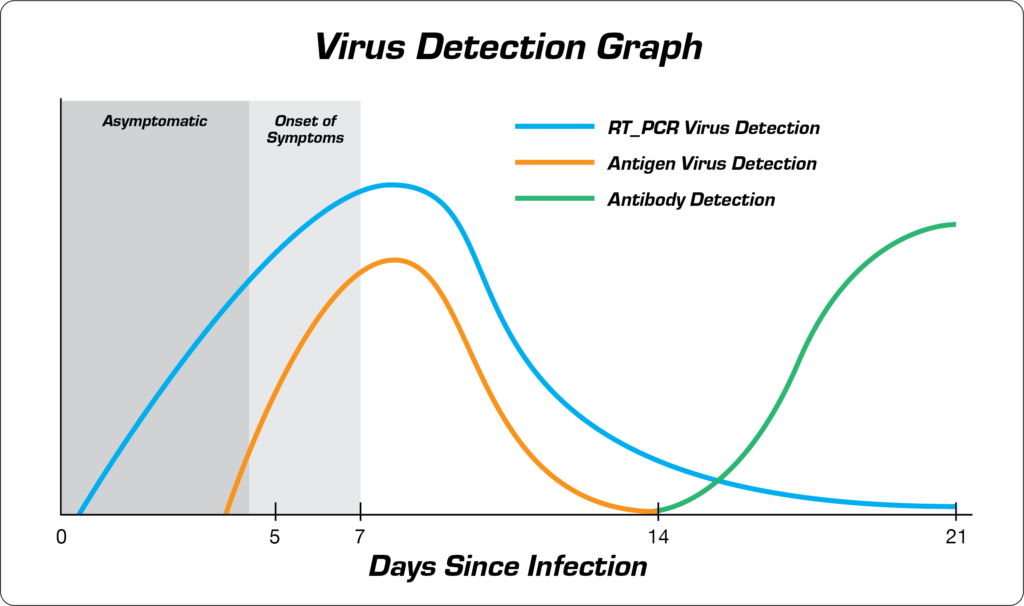
For this reason, antigen tests are not favored by the FDA as a single test for active infection and they suggest an additional molecular test be taken when receiving a negative result from an antigen test*. However, since the antigen testing is quicker and requires less complex technology to perform than molecular testing, frequently repeated antigen testing is considered an acceptable strategy. And like molecular testing, the false positive rate of an antigen test is near zero, so positive results from an antigen test are much more reliable than a negative result.
The technology involved in antigen testing is similar to a pregnancy test or a rapid strep test, so results are usually available in less than 15 minutes. Rapid antigen testing is good way to quickly identify if someone has a positive infection so that quarantining and contact tracing can begin sooner.
How can we help?
Pro Safety & Rescue is here to assist you and your company in preventing a Coronavirus outbreak and can provide large-scale rapid antigen and RT-PCR testing at your location. Contact us to find out more.
Testing for Past Infection
Antibody tests (also called serologic testing)
Antibody tests require blood to be drawn from the patient by a certified phlebotomist and must be done at a doctor’s office, a testing lab, or hospital.
These blood tests identify antibodies that the host body’s immune system has produced in response to the infection. While a serologic test cannot tell you if you are currently infected with the virus, it can accurately identify a past infection.
Results of a Serologic test are usually available within a few days, however, having an antibody test done too early can also lead to a false negative result because it usually takes a week or two after an infection for the host body’s immune system to produce antibodies. And while a positive serologic test proves that the patient has been exposed to the virus, it’s not yet known whether such results indicate a lack of future contagiousness, or the existence of any long-lasting protective immunity.
The Verdict
Deciding which test is best for you can be confusing, because the options are rapidly changing. As previously mentioned, evidence shows the molecular RT-PCR test to be the gold standard accepted by the FDA and most entities seeking a confirmed negative result. However, a regular schedule of antigen testing can be an alternative strategy for your workplace. Our team is dedicated to staying on the forefront of COVID testing and are ready 24/7 to assist you and your company in being pro-active to maintain proper health and safety for you, your employees, and your clients. Contact us to schedule a consultation. 888.269.5095
Much of this content was sourced from Robert H. Shmerling, MD, Senior Faculty Editor, Harvard Health Publishing.https://www.health.harvard.edu/blog/which-test-is-best-for-covid-19-2020081020734
For more information about coronavirus and COVID-19, see the Harvard Health Publishing Coronavirus Resource Center.
Graph adapted from data presented by SYNLAB
https://www.synlab.com/news-publications/sars-cov-2/antigen-tests-for-sars-cov-2-detection
and America’s ER
https://americaser.com/covid19/
*Coronavirus Disease 2019 Testing Basics pamphlet from the FDA https://www.fda.gov/media/140161/download
